
HSCT conditioning varies in the degree of myelosuppression and immune suppression from high-dose myeloablative to reduced intensity conditioning (RIC). First, recipient HSCs must be depleted to create niche space for incoming donor HSCs, and second, the transplanted cells must escape immune rejection by the recipient. For engraftment of allogeneic or gene corrected autologous HSCs, two obstacles must be overcome. Although HSCT is most often performed for the treatment of malignancies, HSCT has been successfully employed as treatment of nonmalignant lymphohematological disorders such as thalassemia, sickle cell anemia, aplastic anemia, inherited immunodeficiencies, autoimmune diseases, and metabolic storage disorders ( 2– 10) and for tolerance induction in transplant patients receiving solid organ grafts ( 11, 12). Hematopoietic stem cell transplantation (HSCT) is an effective treatment modality that enables replacement of host HSCs with HSCs from a healthy donor or genetically corrected HSCs from the patient ( 1). Hematopoietic stem cells (HSCs) replenish the blood system throughout the life span of an organism and maintain homeostasis. The purpose of the current review is to discuss the literature exploring antibody-based conditioning that includes native antibody, radiolabeled antibody conjugates, and ADC for allo-HSCT. Antibody-drug-conjugate (ADC) combined with reduced intensity conditioning or high dose ADC as single dose monotherapy have shown promise for allo-HSCT in preclinical models. Recently, several novel proof-of-concept antibody-mediated preconditioning methods have been developed that can selectively target hematopoietic stem and immune cells with minimal overall toxicity. Under these conditions, mixed chimerism and transplantation tolerance to fully MHC mismatched donor marrow was observed. An alternative approach to allo-HSCT has been developed and tested in preclinical mouse models in which nonmyeloablative preconditioning with low dose of the alkylating agent (busulfan) or lower systemic dose of irradiation combined with co-stimulatory pathway blockade (CTLA4-Ig, anti-CD40L monoclonal antibody) and/or immunosuppressive drugs have been used. ROIC clinical data provide evidence for decreased relapse without increased transplant-related mortality by delivering higher targeted radiation to sites of malignancy than when given in a nontargeted fashion. 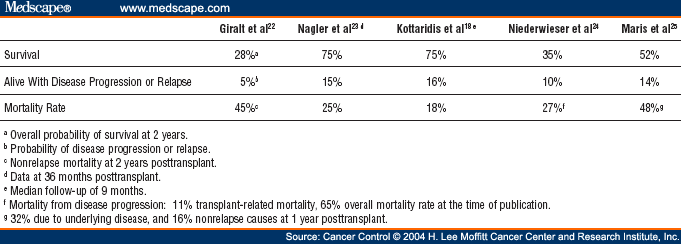 
The delivery of targeted radiotherapy to hematopoietic tissues with the use of a radioimmunoconjugate (ROIC) as a part of transplant preparative regimen has shown clinical benefits. However, these procedures also result in nonspecific tissue injury that can cause short- and long-term adverse effects as well as incite and amplify graft-versus-host-disease (GVHD). Conventional allo-HSCT requires high dose of irradiation and/or chemotherapy to produce sufficient host stem cell and immune system ablation to permit donor HSC engraftment. To achieve stable engraftment of donor hematopoietic stem cells (HSCs), recipient HSC deletion is needed to create space for incoming donor HSCs and donor HSCs must escape immune rejection by the recipient. 2Department of Pediatrics, University of Minnesota, Minneapolis, MN, United StatesĪllogeneic hematopoietic stem cell transplantation (allo-HSCT) is a curative therapeutic option for many patients with hematological malignancies and nonmalignant hematopoietic disorders.1Division of Blood & Marrow Transplant & Cellular Therapy, Masonic Cancer Center, University of Minnesota, Minneapolis, MN, United States.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
